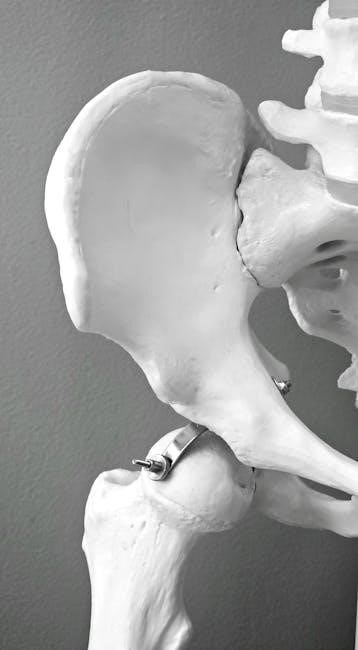
Pelvic Floor Manual Therapy: A Comprehensive Overview
Pelvic floor manual therapy utilizes hands-on techniques to address dysfunction‚ improving muscle relaxation and lengthening through internal and external assessments.
Pelvic floor dysfunction encompasses a range of conditions affecting the muscles and tissues supporting the pelvic organs. These dysfunctions can manifest as urinary or fecal incontinence‚ pelvic organ prolapse‚ and pelvic pain‚ significantly impacting quality of life. Often‚ individuals experience tenderness or discomfort within the pelvic floor muscles themselves‚ contributing to these issues.
Traditional treatments have often focused on exercises alone‚ but a growing body of evidence highlights the benefits of a more holistic approach. This is where pelvic floor manual therapy emerges as a valuable intervention. Therapists utilize skilled hands-on techniques to assess and address restrictions within the myofascial structures and muscles‚ aiming to restore optimal function and alleviate symptoms. Understanding the intricate anatomy and potential causes of dysfunction is crucial for effective treatment.
What is Pelvic Floor Manual Therapy?
Pelvic floor manual therapy is a specialized form of physical therapy employing hands-on techniques to address dysfunction within the pelvic floor muscles and surrounding tissues. Therapists utilize both external and internal methods to assess muscle tension‚ trigger points‚ and myofascial restrictions.
Internal assessment‚ involving gentle vaginal or rectal evaluation‚ allows for direct palpation of pelvic floor muscles‚ identifying areas of tenderness and dysfunction with patient feedback. Techniques like myofascial release‚ muscle energy techniques‚ and trigger point release are then applied to restore muscle length‚ reduce pain‚ and improve overall function. This approach aims to normalize muscle tone‚ enhance pelvic stability‚ and alleviate associated symptoms like incontinence or pain.

Understanding the Pelvic Floor Anatomy
The pelvic floor comprises muscles and fascia supporting pelvic organs‚ crucial for bladder‚ bowel‚ and sexual function; understanding this anatomy is key for therapy.
Key Muscles of the Pelvic Floor
The levator ani muscle group is fundamental‚ encompassing the pubococcygeus‚ iliococcygeus‚ and puborectalis muscles – forming a sling supporting pelvic organs. The pubococcygeus aids in urinary and fecal continence‚ sexual function‚ and pelvic stability.
The iliococcygeus supports the pelvic viscera and contributes to pelvic floor stability‚ while the puborectalis acts as a sling around the rectum‚ controlling bowel movements.
The coccygeus muscle‚ smaller but significant‚ provides additional pelvic floor support. These muscles work synergistically‚ and dysfunction in one can impact the entire system; Accurate assessment and targeted manual therapy are vital for restoring optimal function and addressing related issues like incontinence or pelvic pain.
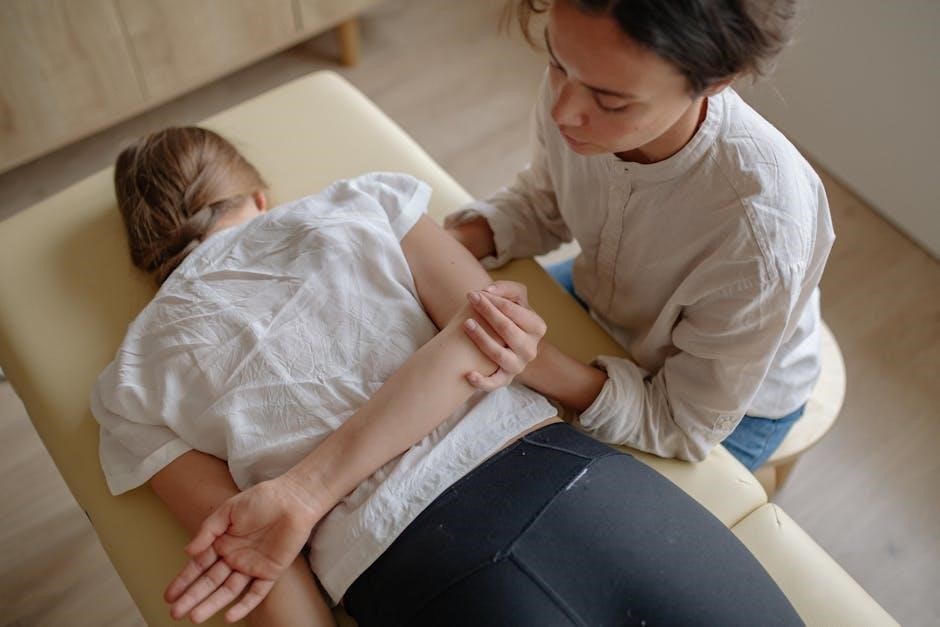
Myofascial Structures and Their Function
Myofascial structures within the perineum and pelvic floor – including fascia‚ ligaments‚ and connective tissues – provide crucial support and transmit forces throughout the pelvis. These structures envelop and interconnect the pelvic floor muscles‚ influencing their function and coordination.
Injury or dysfunction within these tissues can lead to restrictions‚ pain‚ and altered biomechanics‚ impacting pelvic organ support and contributing to conditions like pelvic girdle dysfunction.
Myofascial release techniques aim to address these restrictions‚ restoring tissue mobility and reducing pain. Current literature emphasizes the interconnectedness of the myofascial system‚ highlighting the importance of a holistic approach to treatment‚ considering the influence of surrounding tissues on pelvic floor health.

Assessment Techniques in Pelvic Floor Manual Therapy
Assessment involves external palpation and‚ crucially‚ internal techniques – vaginal or rectal – to identify muscle tenderness and dysfunction with patient feedback.
External Palpation and Assessment
External palpation forms a vital initial step in pelvic floor assessment‚ allowing the therapist to evaluate superficial muscle tone and identify areas of tenderness or trigger points. This involves gentle pressing and assessing the lower abdomen‚ inner thighs‚ gluteal muscles‚ and the perineum itself.
The therapist observes for asymmetries‚ muscle guarding‚ and skin texture changes. Assessing the pelvic girdle’s movement and stability is also crucial‚ as dysfunction here often contributes to pelvic floor issues. Observing the patient’s posture and gait provides further clues about muscle imbalances.
This external examination helps establish a baseline and guides the need for‚ and focus of‚ more detailed internal assessment. It’s a non-invasive way to gather valuable information before proceeding with internal techniques.
Internal Assessment: Vaginal and Rectal Techniques
Internal assessment‚ utilizing vaginal or rectal palpation‚ allows for direct evaluation of pelvic floor muscle function‚ strength‚ and tenderness. A gloved finger gently assesses muscle contractions‚ resting tone‚ and identifies specific areas of discomfort reported by the patient.
This technique evaluates the levator ani muscle‚ endopelvic fascia‚ and surrounding structures. Assessing the ability to contract and relax the pelvic floor muscles is key. The therapist notes any hypertonicity (overactivity) or hypotonicity (weakness).
Biofeedback devices can be incorporated during internal assessment to provide objective data on muscle activity. Patient feedback is crucial throughout the process‚ ensuring comfort and accurate identification of problem areas.

Manual Therapy Techniques for Pelvic Floor Dysfunction
Manual therapy employs myofascial release‚ muscle energy techniques‚ and trigger point release to restore pelvic floor muscle function and alleviate associated pain.
Myofascial Release Techniques
Myofascial release addresses restrictions within the pelvic floor’s connective tissues‚ aiming to restore optimal length and mobility. Therapists gently apply sustained pressure to the myofascial structures‚ releasing tension and improving tissue glide. This technique targets the perineum and surrounding areas‚ addressing potential dysfunctions stemming from injury or chronic tension.
The goal is to release fascial adhesions that can contribute to pelvic pain‚ incontinence‚ and organ prolapse. By restoring the natural length and movement of the fascia‚ myofascial release can improve pelvic floor muscle function and reduce discomfort. Patient feedback is crucial during the process‚ ensuring a comfortable and effective treatment experience. This hands-on approach complements other pelvic floor therapies.
Muscle Energy Techniques (MET)
Muscle Energy Techniques (MET) utilize gentle muscular contractions by the patient‚ against a precisely controlled counterforce applied by the therapist‚ to restore pelvic floor muscle balance. This approach aims to lengthen shortened muscles and strengthen inhibited ones‚ improving overall pelvic floor function.
MET involves specific positioning and controlled contractions‚ allowing for a normalized resting muscle length. It’s particularly effective for addressing muscle imbalances contributing to pelvic pain or dysfunction. The technique relies on the patient’s active participation‚ enhancing proprioception and neuromuscular control. MET can address restrictions in the pelvic girdle and improve coordination between pelvic floor muscles and surrounding structures‚ leading to improved stability and reduced discomfort.
Trigger Point Release
Trigger Point Release focuses on identifying and deactivating hypersensitive spots within the pelvic floor muscles‚ known as trigger points. These points can cause referred pain patterns‚ muscle tension‚ and limited range of motion. Manual pressure is applied to these trigger points‚ sustained until a release is felt by both the therapist and patient.
This technique aims to reduce muscle spasm‚ alleviate pain‚ and restore normal muscle function. Trigger point release can be performed both externally and internally‚ depending on the location of the trigger point and patient comfort. It’s often combined with other manual therapy techniques for a comprehensive approach. Successfully releasing trigger points improves pelvic floor muscle coordination and reduces overall pelvic discomfort‚ enhancing patient well-being.

Conditions Treated with Pelvic Floor Manual Therapy
Pelvic floor manual therapy effectively addresses pelvic organ prolapse‚ urinary/fecal incontinence‚ and pelvic girdle dysfunction‚ providing pain relief and improved function.
Pelvic Organ Prolapse Management
Pelvic organ prolapse occurs when pelvic organs descend from their natural position‚ often due to weakened pelvic floor muscles. Manual therapy plays a crucial role in management by addressing contributing factors like myofascial restrictions and muscle imbalances. Therapists utilize both external and internal techniques – vaginal or rectal – to assess muscle tone and identify areas of tenderness or dysfunction.

Treatment focuses on restoring optimal muscle function‚ improving support for the prolapsed organs‚ and reducing associated symptoms such as pressure or discomfort. Myofascial release can address tissue restrictions‚ while muscle energy techniques help to re-educate and strengthen the pelvic floor. Importantly‚ pelvic floor muscle training (Kegels) is often integrated with manual therapy to enhance long-term results‚ offering a non-invasive approach to improve quality of life.
Urinary and Fecal Incontinence Treatment
Urinary and fecal incontinence often stem from weakened pelvic floor muscles or dysfunction‚ impacting bladder and bowel control. Pelvic floor manual therapy offers a targeted approach to address these issues‚ focusing on restoring muscle strength‚ coordination‚ and function. Therapists employ both external palpation and internal techniques – vaginal or rectal – to assess muscle tone‚ identify trigger points‚ and evaluate myofascial restrictions.
Myofascial release helps alleviate tissue tension‚ while muscle energy techniques aim to re-educate and strengthen the pelvic floor. Integrating biofeedback can enhance patient awareness and control. This combined approach‚ alongside targeted pelvic floor muscle exercises (Kegels)‚ provides a comprehensive‚ non-invasive treatment option‚ improving continence and enhancing overall pelvic health and quality of life.
Pelvic Girdle Dysfunction and Pain Relief
Pelvic girdle dysfunction (PGD) frequently presents with pain in the lower back‚ hips‚ and pelvis‚ often linked to imbalances within the pelvic floor muscles and surrounding myofascial structures. Pelvic floor manual therapy addresses these connections‚ utilizing techniques to release tension and restore optimal biomechanics. Therapists apply hands-on methods to address muscle imbalances‚ trigger points‚ and fascial restrictions impacting the pelvic girdle.
Current literature emphasizes the importance of a myofascial approach‚ recognizing the interconnectedness of tissues. Myofascial release and muscle energy techniques are key components‚ improving pelvic alignment and reducing pain. This holistic treatment‚ combined with targeted exercises‚ aims to restore function‚ alleviate discomfort‚ and improve overall pelvic stability‚ enhancing a patient’s quality of life.

The Role of Pelvic Floor Muscle Training (Kegels)
Pelvic floor muscle training (Kegels)‚ often combined with manual therapy‚ strengthens muscles and improves function‚ aiding in prolapse management and incontinence treatment.
Integrating Kegels with Manual Therapy
Combining Kegel exercises with pelvic floor manual therapy offers a synergistic approach to treatment‚ maximizing positive outcomes for patients experiencing dysfunction. Manual therapy first addresses myofascial restrictions and muscle imbalances‚ creating an optimal foundation for effective muscle retraining.
If muscles are tight or tender‚ simply contracting them with Kegels can exacerbate the problem. Manual techniques release this tension‚ allowing for proper recruitment and strengthening. Furthermore‚ biofeedback can be incorporated to enhance patient awareness and ensure correct technique during Kegel performance.
This integrated strategy isn’t just about strengthening; it’s about restoring coordinated muscle function‚ improving pelvic stability‚ and ultimately‚ enhancing a patient’s quality of life. A tailored program‚ guided by a skilled therapist‚ is crucial for success.
Biofeedback and Pelvic Floor Rehabilitation
Biofeedback plays a vital role in pelvic floor rehabilitation‚ providing patients with real-time visual or auditory feedback on muscle activity. This empowers them to understand and control their pelvic floor muscles more effectively‚ enhancing the benefits of manual therapy and targeted exercises. Devices can be inserted vaginally or rectally to monitor muscle contractions.
It’s particularly useful for individuals who struggle to identify or properly engage their pelvic floor muscles. Biofeedback helps bridge the gap between intention and execution‚ ensuring correct technique and maximizing the effectiveness of Kegel exercises.
Combined with manual therapy‚ biofeedback creates a comprehensive rehabilitation program‚ addressing both structural and neuromuscular components of pelvic floor dysfunction‚ leading to improved outcomes and lasting relief.
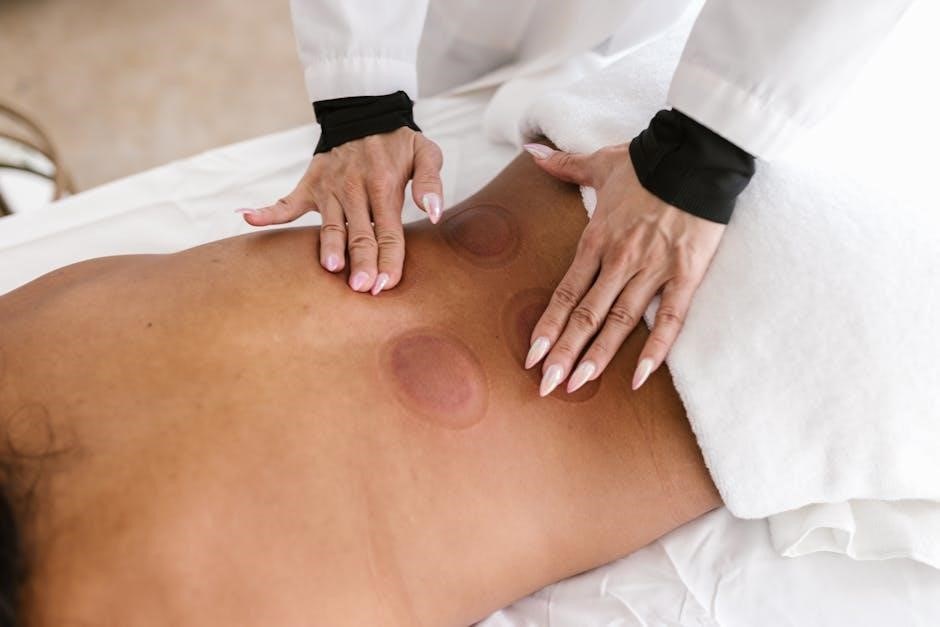
Current Research and Clinical Effectiveness
Current studies evaluate pelvic floor muscle training’s effectiveness‚ while diagnosis of levator ani injuries utilizes accessible manual techniques for assessment and treatment.
Evaluating the Effectiveness of Pelvic Floor Muscle Training
Pelvic floor muscle training‚ often involving Kegel exercises‚ stands as a prominent non-invasive treatment approach‚ particularly for pelvic organ prolapse. However‚ a definitive consensus regarding its optimal application remains elusive‚ prompting ongoing research. Clinical evaluations aim to determine the extent to which these exercises genuinely improve systemic function and alleviate associated symptoms.
Studies are actively investigating the clinical effectiveness of integrating pelvic floor muscle training within comprehensive treatment plans. Researchers are focused on quantifying improvements in areas like urinary and fecal incontinence‚ pelvic pain‚ and overall pelvic floor stability. The goal is to establish evidence-based guidelines for utilizing these exercises‚ maximizing their benefits for patients experiencing pelvic floor dysfunction. Further investigation is crucial to refine protocols and personalize treatment strategies.
Traumatic Injuries of the Levator Ani Muscle and Diagnosis
Diagnosing traumatic injuries to the levator ani muscle and surrounding fascia relies heavily on accessible and straightforward manual techniques. These methods are crucial for identifying subtle disruptions often missed by standard imaging. Skilled therapists employ palpation and assessment to pinpoint areas of tenderness‚ asymmetry‚ or restricted movement within the pelvic floor.

The diagnostic process involves carefully evaluating muscle function and fascial integrity‚ seeking evidence of tears‚ strains‚ or nerve impingement. These manual assessments‚ combined with patient feedback regarding pain and discomfort‚ allow for a targeted approach to treatment. Early and accurate diagnosis is paramount for initiating appropriate pelvic floor rehabilitation and preventing chronic dysfunction.